According to the American Academy of Implant Dentistry (AAID), 3 million Americans have one or more dental implants. That same report also states that 500,000 more people are added to that number annually.
So, why implant dental is one of the most popular options for fixing missing or damaged teeth? The answer is simple: They are long-lasting, have an incredibly high success rate, and are designed to match your natural teeth.
If you have been considering getting one, you must understand everything there is to know about such oral devices.
This article examines the available types, the benefits such fixtures offer, the associated risks, and what the surgical procedure typically involves.
Read on to know more.
What is a Dental Implant?
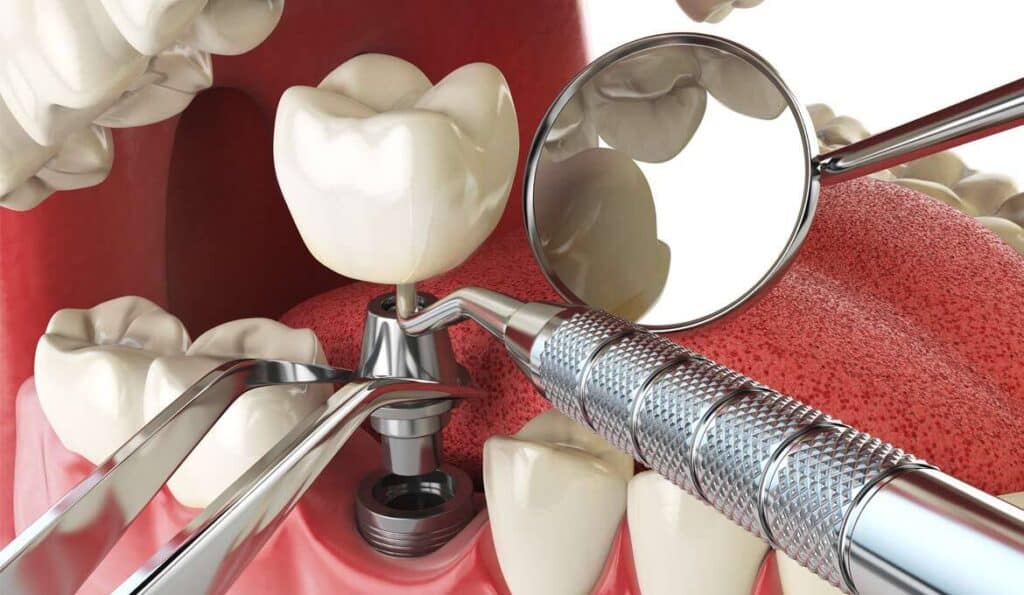
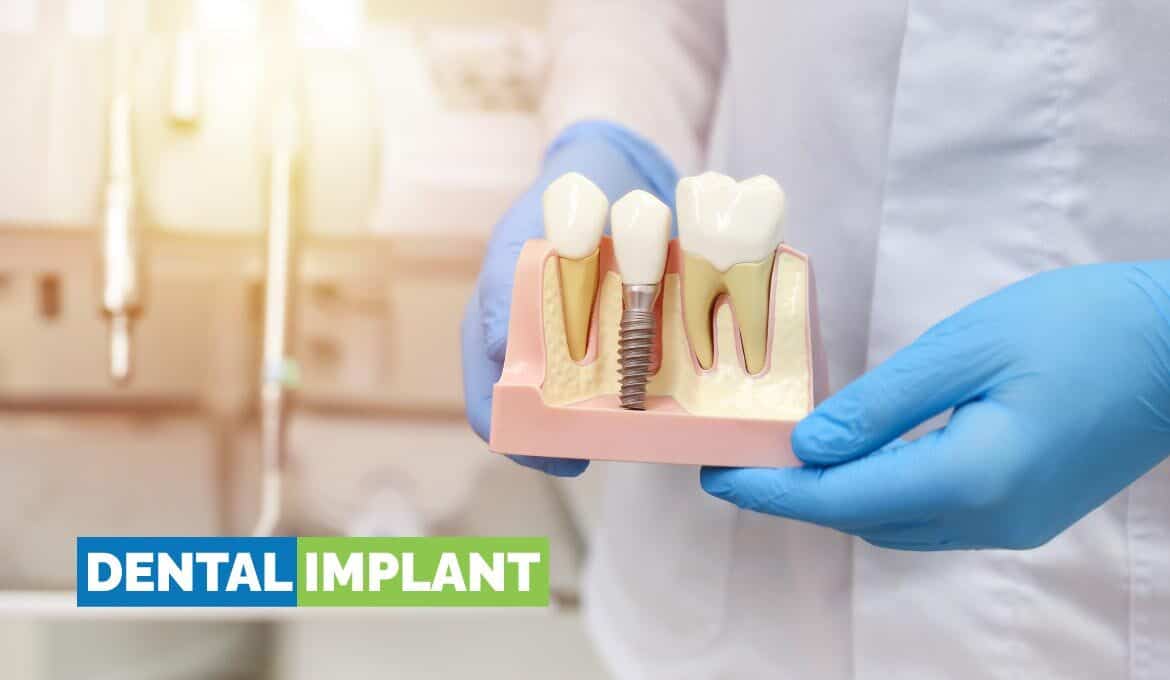
A dental implant is an artificial replacement for a missing or damaged tooth. It consists of an anchor screw (implant post) that is fixed onto the jawbone, with a connective device attaching it to an artificial tooth.
In most cases, dental implants system are custom-made and fitted to match the individual’s natural teeth. In addition, unlike other oral devices, they are designed to be permanent solutions, lasting a lifetime if maintained properly.
Now, depending on how their placement, such oral fixtures are primarily categorized into the following:
- Endosteal: The most commonly opted-for variant, endosteal implants resemble miniature screws and are surgically fixed onto the jawbone. In short, they act as an artificial anchor, replacing damaged tooth roots.
- Subperiosteal: These implants are only recommended when a patient does not have sufficient jawbone density to maintain the implant post. Subsequently, instead of being drilled into the underlying bone, dentists place the post socket directly above or on it.
Note that the classification for the implant types is solely based on the surgical procedure. Neither of the two has any advantage over the other.
What Does Dental Implant Surgery Typically Involve?
A dental implant procedure is spread over multiple phases and can last between 3 to 9 months. While the surgery is conducted in one session, the initial examination and post-op recovery process can take a significant amount of time.
Here is a complete overview of the entire process:
1. Preliminary Dental Examination
Dentists will thoroughly examine your teeth, jawbone, and gums to determine your viability for the procedure.
This primarily involves an assessment of your oral hygiene and, more importantly, whether you have enough jawbone density to sustain the implant. If necessary, in some cases, you may have to undergo additional surgical procedures, such as a bone graft.
Concurrently, any existing issues with your gums need to be addressed first. This includes treating periodontitis or other related gum infections.
Moreover, the number of teeth that need replacement will also influence the scope of a dental implant surgical procedure. The process may take significantly longer if it is more than one tooth.
2. Implant Post Placement
The actual placement of a tooth implant depends entirely on the type you are opting for. For instance, for those who are getting an endosteal implant, the procedure will typically involve:
- Making an incision in the gums to expose the jawbone
- Drilling implant post sockets into the bone prior to placement
In the case of subperiosteal implants, surgeons will not drill into the jawbone and instead place the implant post directly on or above the bone.
Since the artificial tooth is not immediately placed onto the implant, you can request a temporary denture to cover the socket to retain your aesthetic appearance.
3. Osseointegration
Following the placement of a dental implant system, it can take anywhere from 2 to 6 months for the jawbone to heal. This process is known as osseointegration. During this phase, your jawbone will recover from the surgery and grow around the implant, strengthening and securing its position.
Oral surgeons will recommend maintaining dental hygiene to avoid complications, such as bacterial infections, during this process.
4. Abutment Placement
An abutment is a metal extender that connects the implant post to the artificial tooth (crown). In most cases, surgeons will place the abutment while drilling the sockets for the dental implant posts.
However, depending on your preference, a dentist can perform this later through a minor supplementary procedure. The process involves making an incision into the healed gum tissue and then screwing the abutment on top of the implant post.
The post-op recovery, in this instance, can take up to several weeks and result in some swelling and pain.
5. Crown Placement
After the successful placement of the abutment, a dentist will take an impression of your teeth to order a custom-fitted crown.
Here, you can opt for a removable or fixed tooth. In the case of the former, dentists will attach the crown to a metal frame before screwing it on top of the abutment. If you request the latter, the crown will be permanently screwed and cemented onto the abutment.
Once this is complete, your new tooth implant must be cared for and maintained with daily flossing and brushing.
However, consult your dentist if you experience any of the following:
- Bleeding or swelling around the gums
- Uneven bite
- Pain at the implant site
The issues listed above can be indicative of incorrect crown positioning. It is recommended to seek an immediate appointment with a dentist to avoid any additional complications.
Are Dental Implants Safe?
While some question their viability, a dental implant system is safe and has a high success rate when it comes to implantation.
Apart from that, these oral devices offer several other advantages, including:
- A Natural-Looking Appearance: Unlike other dental devices, implants are nearly indistinguishable from your natural teeth, resulting in a more cohesive aesthetic appearance.
- Improved Speech & Comfort: Dentures and other oral fixtures often lead to slurred speech and are relatively uncomfortable to wear for extended durations. Implants, however, are specifically designed to fuse with your jawbone and cause no interference with speech.
- Improved Oral Health: A tooth implant procedure does not require any alterations to the other teeth and is restricted to a specific site. This limit the impact on your overall oral health.
- Durability: A dental implant system is made out of highly durable material, such as titanium. Thus, these oral devices are usually permanent solutions to remedying damaged or infected teeth. In rare instances, a dentist may recommend replacing your crown. However, this will only occur due to severe damage or poor oral hygiene.
In addition to the mentioned benefits, dental implants are suitable for almost everyone. Exceptions are only applicable if the patient has severe gum disease or lacks sufficient jawbone density.
Regardless, dentists can remediate these issues with the appropriate treatment. Following that, the individual in question can opt for the procedure.
Risks & Complications Associated with Dental Implant Surgery
Like all surgical procedures, there are a few risks associated with dental implant surgery. Even so, these complications are rare and avoidable in most cases.
Nonetheless, to convey the necessary information, here are a few cases where a dental implant system can lead to additional problems:
1. Bacterial Infections
Patients who opt for a tooth implant procedure have a small risk of developing bacterial infections. This is often a result of poor oral hygiene in the post-op phase. A bacterial infection can also occur if the gum tissue does not heal properly or grows around the post socket.
As such, if you notice any swelling around your gums, loose teeth, or pus-filled abscesses near the implant site, consult a dentist immediately. Delaying treatment can cause permanent damage to your gum roots and other healthy teeth.
2. Nerve or Sinus Damage
In rare cases, dental implant surgery can cause damage to your facial nerves and sinuses, resulting in a numbing sensation or pain near the operation site. This is most common in patients who opt for implants in their upper teeth. For instance, the post socket may be incorrectly positioned and rupture the blood vessels in the gums.
That is precisely why it is crucial to verify your dentist’s credentials and undergo the surgery from a professional you trust.
3. Implant Rejection
A patient’s body can reject a dental implant. This can happen due to several reasons, including the following:
-
Peri-Implantitis
Also known as peri-implant disease, peri-implantitis is a type of gum infection that occurs due to poor oral hygiene. While rare in individuals without implants, the condition most commonly manifests in patients who have undergone recent dental implant surgery and, subsequently, fail to maintain their oral health.
Signs of peri-implantitis include gum inflammation, bleeding, and severe pain in your jawbone, especially near the implant site. Seek an appointment with your dentist upon experiencing any of those mentioned symptoms.
-
Inhibited Osseointegration
In a few cases, the jawbone may not heal completely after the placement of the implant post. This can be due to peri-implantitis, involuntary teeth grinding, or poor oral hygiene.
Regardless of how it happens, a lack of osseointegration results in the implant post coming loose, preventing the procedure from progressing any further.
To avoid such problems, ensure that you have a thorough discussion with your dentist regarding your medical history and any past episodes of dental issues. This will help them design an implantation process that specifically caters to your requirements and eliminate the common early and late complications associated with such oral fixtures.
What Should You Expect After Undergoing Tooth Implant Surgery?
Usually, tooth implant surgery will result in the following:
- Minor facial and gum swelling
- Pain at the implant site
- Bleeding around the gums
While common, these issues only last for a few days after the surgical procedure. If they persist, it may indicate a more severe underlying problem. Seek an appointment with your dentist in such cases.
In addition, you may have to take antibiotic medication to avoid developing bacterial infections. Doctors can also prescribe pain relievers to patients upon request.
Apart from this, maintain a habit of brushing daily and avoid hard-to-chew foods for the first few weeks since they can damage the implant site.
Wrapping Up
While it is one of the most effective methods to replace missing or damaged teeth, a dental implant does require patients to meet a few specific parameters.
For example, as mentioned previously, you must have the necessary jawbone density and relatively healthy gums.
Besides that, it is advisable to avoid such procedures if you have recently undergone another surgery, oral or otherwise. This is primarily due to how the human body needs time to recover from surgical procedures.
Opting for a subsequent operation immediately after another can leave you vulnerable to bacterial infections.
Consider discussing all of this with your dentist. This will ensure that you understand your suitability for the procedure.
Frequently Asked Questions
1. How much does a tooth implant cost on average?
Since implants are lifetime investments, they tend to be priced slightly higher than other dental devices. In the US, this can be anywhere between $3,000 to $4,500. For those needing implants for multiple teeth, the cost of surgery can range from $60,000 to $90,000. Note that this covers the entirety of the procedure, from a dental examination to crown placement.
2. What can inhibit osseointegration?
Apart from bacterial infections, incorrect implant positioning, peripheral gum tissue damage, and recent radiation therapy can prevent osseointegration. This is why it’s crucial to inform your dentist about your medical history to help improve the chances of a successful implant.
3. How long does it take to recover from dental implant surgery?
Depending on the patient's age, overall health, and oral hygiene standards, complete recovery after a dental implant surgery can take 3-6 months. Regardless, residual pain from the procedure should disappear after a few days. It is advisable to consult your dentist if you face any issues during this period.
4. What are tooth implants made of?
A dental implant system is typically made out of zirconium oxide or titanium. However, ceramic, cobalt-based alloys, and gold-titanium composites are also used in a few instances. These materials are preferred over others due to their safety profiles.
Read Also: