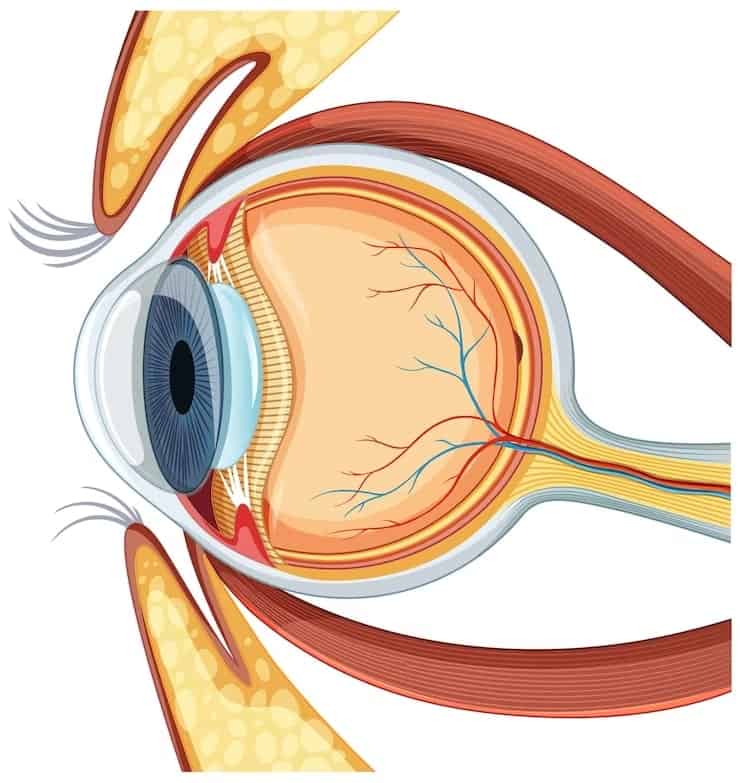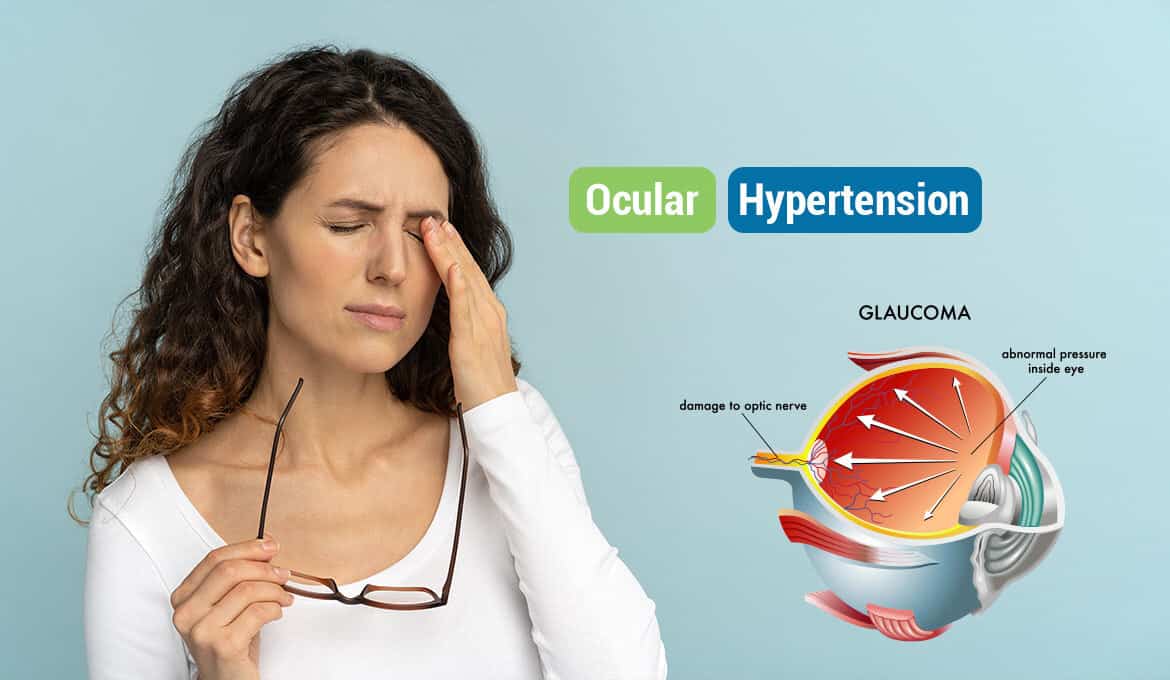
Our intraocular pressure, the pressure inside our eyes, can generally give an overall picture of our eye health. It enables eye doctors to find signs of optic nerve damage in our eyes that may impair our vision.
The normal intraocular pressure changes daily and varies from person to person. However, in healthy eyes, a certain fluid, which fills our eyes to keep them inflated like a ball, drains freely to keep eye pressure steady.
If the pressure inside the eye is higher than normal, one may suffer from ocular hypertension. It isn’t a disease, but it can likely develop into glaucoma, a group of eye diseases that damage the optic nerve, causing vision loss and blindness.
Symptoms
The tricky side of ocular hypertension is that it doesn’t have noticeable signs or symptoms. While certain eye problems cause headaches or dizziness, they don’t usually happen with ocular hypertension.
That’s why it’s essential to consult your healthcare provider and take regular eye exams to check if the pressure inside your eye is high. If the pressure is too high, you may feel eye pain with the movement or touching of your eyes.
Causes
As mentioned earlier, there’s a particular fluid that flows in and out the front of our eyes. It’s called “aqueous humor.” Our eyes continually make it and drain an equal amount of it out of our eyes to maintain a constant healthy intraocular pressure or eye pressure.
Intraocular pressure can be measured in millimeters of mercury (mmHg). Normal eye pressure ranges from 10-21 mmHg. However, if aqueous humor doesn’t flow out of our eyes properly, pressure will build up higher than 21 mmHg and cause ocular hypertension.
If ocular hypertension persists, the high eye pressure can result in optic nerve damage and may lead to glaucoma, which causes vision loss.
Risk Factors
In the United States, around 3 million people suffered from glaucoma as of 2022, and approximately 120,000 of this number became legally blind. These figures emphasize the need to characterize those people who are likely to develop glaucoma, particularly those with ocular hypertension.
Anyone can suffer from ocular hypertension, but certain people are more likely to get this condition. They include people who:
- Are hypertensive (with high blood pressure);
- Are very myopic (nearsighted);
- Are diabetic;
- Have a family history of ocular hypertension or glaucoma;
- Take long-term steroid medications;
- Suffered from eye injuries or surgery; or
- Have pseudoexfoliation syndrome (PXF), commonly called pigment dispersion syndrome.
Additionally, according to several studies over the last 20 years, the following are risk factors for ocular hypertension and glaucoma development:
- People over age 40 are likely to develop glaucoma for the next five years. They have an average risk of 10%. On a positive note, they can have a 50% decrease in risk if their eye pressure is reduced by medications or laser surgery. It can even be less than 1% per year, thanks to the advancements in detecting glaucomatous damage.
- People with eye pressure higher than 30 mmHg have a 42% incidence of glaucomatous damage.
- People with thin corneas may have a higher risk for glaucoma development.
- African Americans tend to have thinner corneas. Hence, they’re at a five times greater risk of developing glaucoma than whites. They’re also three to four times more likely to develop open-angle glaucoma, the most common form of glaucoma. It happens when other parts of the drainage system in our eyes don’t drain properly, causing a slow yet progressive increase in eye pressure.
- Women, especially after menopause, may be at a higher risk for ocular hypertension.
- Men with ocular hypertension are likely to suffer from glaucomatous damage.
Diagnosis
Your eye doctor will measure your intraocular pressure and rule out early primary or secondary causes of glaucoma. Specifically, they’ll generally check your:
- Visual acuity, or how well you can read things by having you read letters or numbers from across a room through an eye chart;
- The front of your eyes using a slit lamp, a special microscope for the eye; and
- Eye pressure through the diagnostic test tonometry and using a tonometer to measure how your cornea resists small pressure, which helps determine your eye pressure;
- Dilation of your pupils by taking pictures of the front surface of your optic nerve (or your optic disk) to examine for any damage or abnormalities; and
- The drainage angle of your eye through gonioscopy to rule out any other conditions that may cause high intraocular pressure.
Other doctors also perform visual field testing through an automated visual field machine. This checks your side (or peripheral) vision and determines any visual field defects due to glaucoma. They might also run a pachymetry test to ensure the accuracy of your intraocular pressure readings.
During your eye check-up, ask the following questions to your eye doctor:
- Is my eye pressure high?
- Do I have signs of eye damage due to injuries?
- Is my optic nerve damaged?
- Is my side (or peripheral) vision normal?
- Do I need treatment?
- How often should I visit you for follow-up examinations?
- How much will the treatment cost?
Treatment
Your treatment is highly individualized. Doctors may recommend you be under observation or medication. They’ll discuss the pros and cons of observation versus medical treatment with you; hence consultation with them is necessary.
Overall, medical treatment aims to lower eye pressure before it results in glaucomatous loss of vision. The most common medicine for this is Latanoprost, a generic prescription drug used to lower eye pressure by improving the fluid draining inside the eye.
Latanoprost is a topical medicine, specifically an eye drop. It’s considered a Tier 1 drug and often covered by commercial health insurance.
However, without health insurance coverage, people may have to pay around $77 per 2.5 mL bottle (usually 80 drops or doses, depending on the usage). Fortunately, you can use a Latanoprost Coupon to make it more affordable.
Final Thoughts
Although Latanoprost is a moderately-priced prescription drug, don’t settle for natural remedies, over-the-counter medications, or dietary supplements without a doctor’s advice.
Intraocular hypertension may not be an illness, but it’s a serious condition that can cause blindness. Instead of these risky substitutes, opt for savings cards and shop around for other affordable “prescribed” options.
Read Also: